How does plasminogen activator inhibitor (PAI) regulate fibrinolysis and what are the clinical implications of PAI deficiency or excess?
Published on 02/13/2025 · 7 min readFibrinolysis, the process of breaking down blood clots, is a crucial part of hemostasis. Plasminogen activator inhibitor (PAI) plays a vital role in regulating this process. Understanding PAI's function and its clinical implications is essential for comprehending bleeding and coagulation disorders.
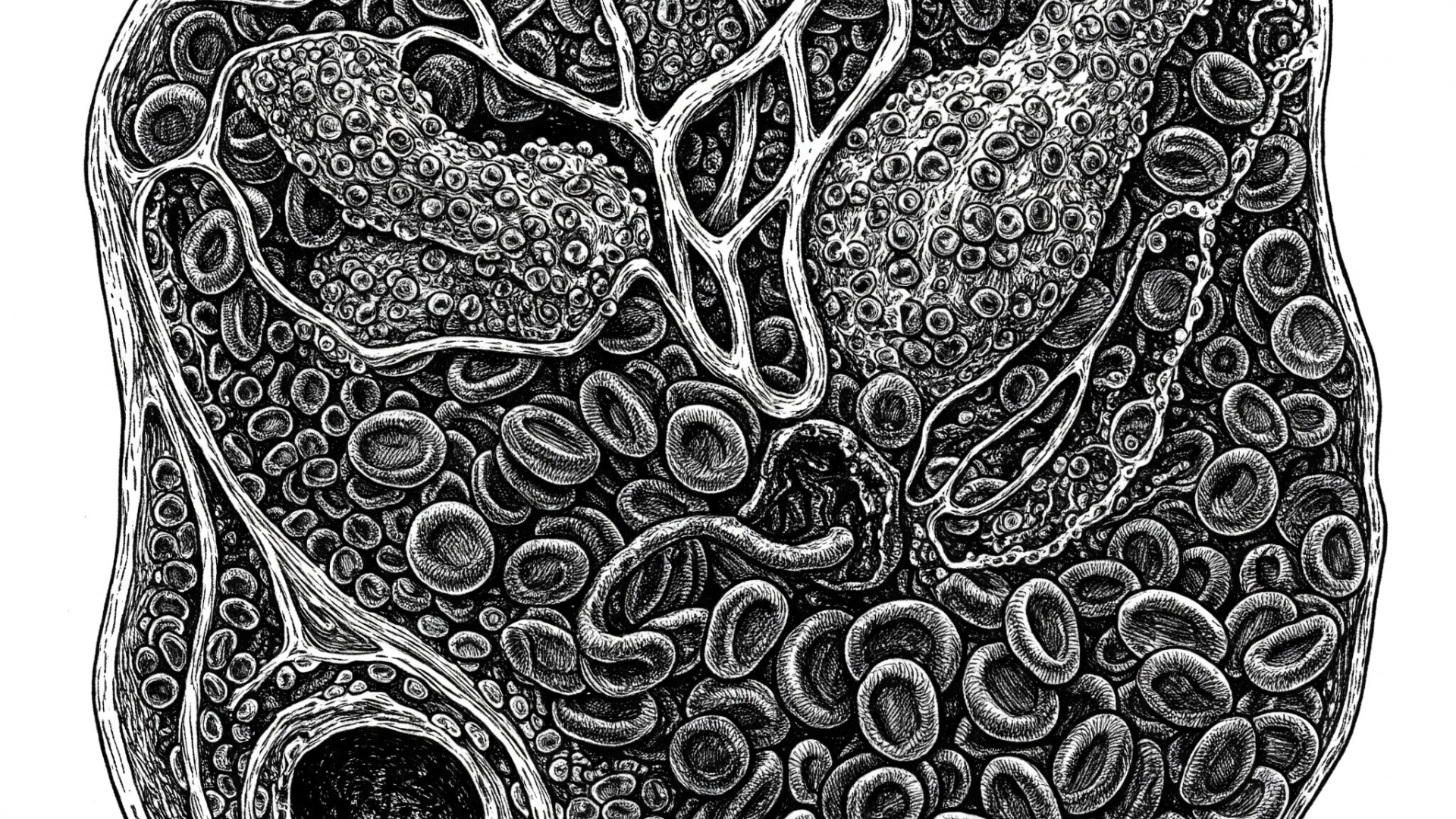
Table of Contents
Understanding Fibrinolysis and PAIThe Process of FibrinolysisThe Role of Plasminogen Activator Inhibitor (PAI)Regulation of FibrinolysisClinical Implications of PAIPAI DeficiencyPAI ExcessPAI-1 and AtherosclerosisClinical PearlsCitations
Understanding Fibrinolysis and PAI
The Process of Fibrinolysis
Fibrinolysis involves the conversion of plasminogen to plasmin, which then degrades fibrin, the protein that forms blood clots. Tissue plasminogen activator (tPA) and urokinase-type plasminogen activator (uPA) are key enzymes that activate plasminogen. [1]
The Role of Plasminogen Activator Inhibitor (PAI)
PAI, specifically PAI-1 and PAI-2, inhibits the activity of tPA and uPA, thereby regulating fibrinolysis. PAI-1 is primarily secreted by endothelial cells and adipose tissue, while PAI-2 is produced by the placenta. [2]
Regulation of Fibrinolysis
Fibrinolysis is tightly regulated to prevent excessive clot formation or excessive bleeding. In addition to PAI, alpha-2-antiplasmin and thrombin-activatable fibrinolysis inhibitor (TAFI) also play roles in this regulation. [3]
Clinical Implications of PAI
PAI Deficiency
A deficiency in PAI can lead to excessive fibrinolysis, resulting in bleeding disorders or hemorrhagic diathesis. This occurs because the inhibition of tPA and uPA is reduced, allowing for increased plasmin activity. [4]
PAI Excess
Conversely, an excess of PAI can lead to decreased fibrinolysis, increasing the risk of thrombosis and atherosclerosis. Conditions such as cancer, obesity, and metabolic syndrome are often associated with elevated PAI levels. [5]
PAI-1 and Atherosclerosis
Elevated PAI-1 levels are specifically linked to an increased risk of atherosclerosis, the hardening of arteries. This is due to the reduced ability to break down clots, contributing to plaque formation. [6]
Clinical Pearls
- PAI deficiency: Increased risk of bleeding.
- PAI excess: Increased risk of thrombosis and atherosclerosis.
- Conditions like cancer, obesity, and metabolic syndrome can elevate PAI levels.
- PAI-1 specifically contributes to atherosclerosis.
Understanding the balance of fibrinolysis and the role of PAI is crucial for diagnosing and managing bleeding and thrombotic disorders.
Citations
[1] Castellino FJ. Plasminogen and plasminogen activation. Methods Enzymol. 1981;80 Pt A:365-78.
[2] Erickson LA, Schleef RR, Ny T, Mullenix C, Lundgren RC. A specific inhibitor of tissue-type plasminogen activator from human endothelial cells. J Biol Chem. 1986;261(10):4312-8.
[3] Bajzar L. Thrombin-activatable fibrinolysis inhibitor. J Thromb Haemost. 2004;2(4):494-500.
[4] Fay WP, Shapiro AD, Shih JL, Schleef RR. Congenital deficiency of plasminogen-activator inhibitor-1 associated with a novel hereditary hemorrhagic syndrome. J Clin Invest. 1992;90(5):1589-96.
[5] Alessi MC, Juhan-Vague I. PAI-1, obesity, insulin resistance and risk of cardiovascular events. Atherosclerosis. 2006;189(1):1-7.
[6] Reilly MP, Iqbal A, Schmaier AH, et al. Toll-like receptor 4 mediates oxidized LDL-induced PAI-1 expression in human macrophages. J Clin Invest. 2003;111(10):1513-21.
Shop related blood tests

Plasminogen Activator Inhibitor-1 (PAI-1)
This test directly measures the level of PAI-1 in the blood, which is crucial for determining the risk of thrombosis and atherosclerosis. Elevated PAI-1 indicates decreased fibrinolysis.

Partial Thromboplastin Time, Activated (aPTT)
While not directly measuring fibrinolysis, aPTT assesses the intrinsic coagulation pathway, which is interconnected with fibrinolysis. Changes in aPTT can indicate abnormalities in the coagulation system, which can secondarily influence fibrinolysis.
Read next
 Written on 02/28/2025
Written on 02/28/2025Sequence vs. Syndrome vs. Association: Understanding Key Medical Terminology?
Ever get tripped up by medical terms like sequence, syndrome, and association? You're not alone! These words describe how different health conditions can occur together, but they each have a distinct meaning. Let's break it down. Read more
 Written on 02/13/2025
Written on 02/13/2025How does plasminogen activator inhibitor (PAI) regulate fibrinolysis and what are the clinical implications of PAI deficiency or excess?
Fibrinolysis, the process of breaking down blood clots, is a crucial part of hemostasis. Plasminogen activator inhibitor (PAI) plays a vital role in regulating this process. Understanding PAI's function and its clinical implications is essential for comprehending bleeding and coagulation disorders. Read more
 Written on 01/15/2025
Written on 01/15/2025How Does the Hardy-Weinberg Principle Calculate Allele and Genotype Frequencies in a Population?
Understanding the genetic makeup of populations is crucial in biology. The Hardy-Weinberg principle provides a mathematical framework to determine allele and genotype frequencies. Let’s break down how this principle works. Read more
 Written on 03/05/2025
Written on 03/05/2025How Do Ventilation and Perfusion Differ Across Lung Zones, and What Are the Implications of V/Q Mismatch in Respiratory Health and Disease?
Understanding how air and blood flow work together in your lungs is key to grasping respiratory health. This post dives into the concepts of ventilation (air in) and perfusion (blood flow) in the lungs, exploring how they vary and why these differences matter. Read more

