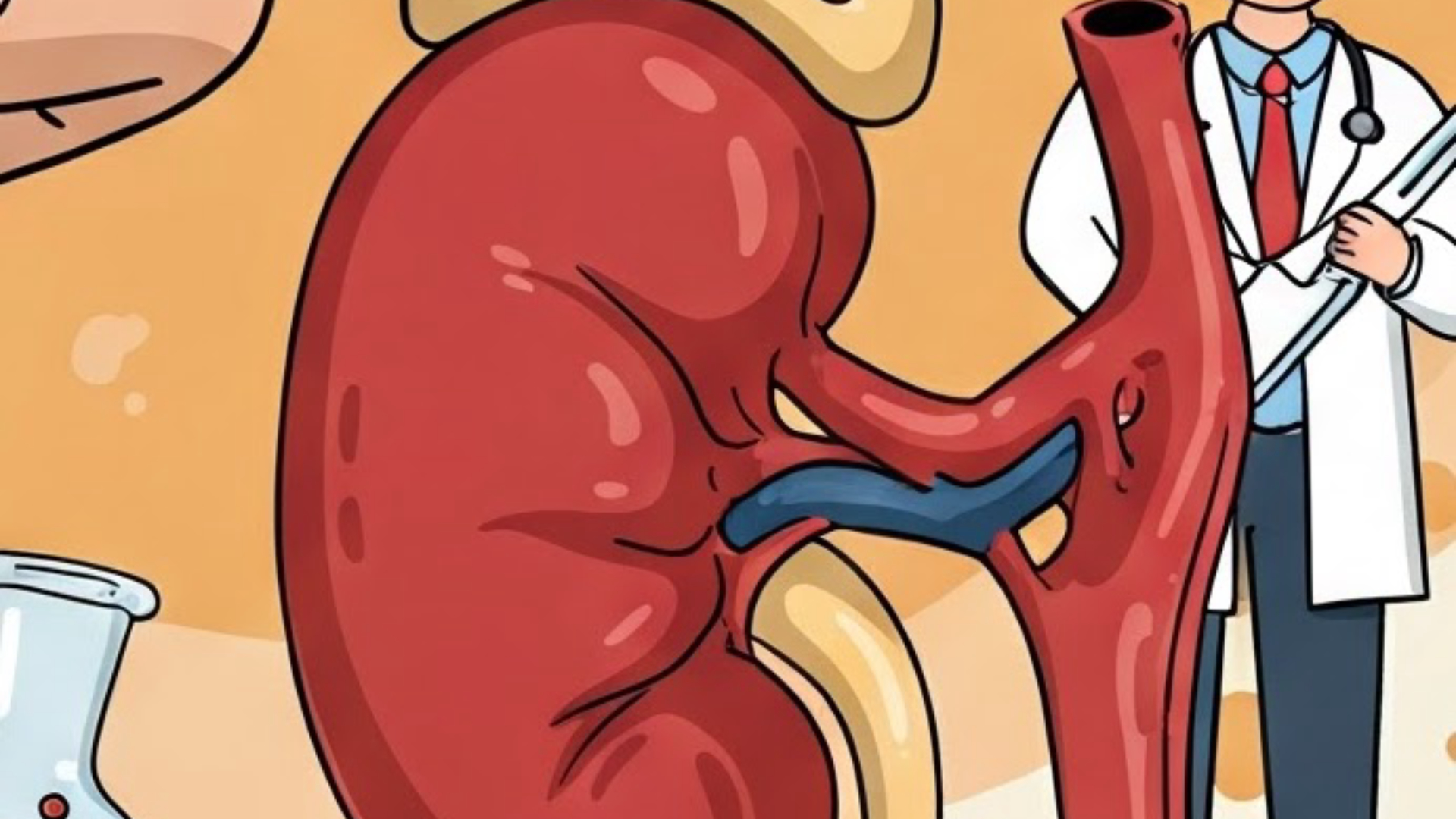
What is Hepatorenal Syndrome? Understanding the Liver-Kidney Connection, Symptoms, and the Role of Vasodilation and Renin?
Published on 03/03/2025 · 6 min readLet's dive into hepatorenal syndrome, a serious condition where a problem in the liver leads to kidney dysfunction. As the name suggests, hepato refers to the liver, and renal refers to the kidney. Understanding this connection is crucial for recognizing and managing this syndrome.
Table of Contents
The Liver's Role in Hepatorenal SyndromeVasodilation and HypotensionThe Heart's ResponseThe Kidneys Under PressureThe Glomerular Response: Renin to the Rescue (or Not?)The Two Actions of ReninConsequences of Hepatorenal Syndrome
The Liver's Role in Hepatorenal Syndrome
The trouble begins in the liver. Whether it's due to cirrhosis, fulminant liver failure, or other severe liver damage, the compromised liver can release excessive amounts of vasodilator substances, notably nitric oxide.
Vasodilation and Hypotension
This overproduction of nitric oxide causes widespread vasodilation, meaning the blood vessels relax and widen. This vasodilation leads to a significant drop in blood pressure, a condition known as hypotension.
The Heart's Response
In response to this drop in blood pressure, the heart tries to compensate by increasing the speed of circulation. This can be somewhat similar to what happens in high-output cardiac failure.
The Kidneys Under Pressure
The kidneys are highly sensitive to changes in blood pressure. When the blood pressure entering the kidneys through the abdominal aorta and renal artery decreases due to systemic hypotension, the kidneys suffer. Think of it this way: a kidney without adequate blood pressure is like a fish out of water.
The Glomerular Response: Renin to the Rescue (or Not?)
Zooming in on a kidney filtering unit, the glomerulus, we see the afferent arteriole bringing blood in and the efferent arteriole taking blood out. When the kidney senses a decrease in blood flow through the afferent arteriole, it triggers the renin-angiotensin-aldosterone system (RAAS).
The Two Actions of Renin
- Salt and Water Reabsorption: Renin initiates a cascade that leads to increased reabsorption of salt and water by the kidneys. This contributes to fluid retention, often manifesting as ascites (fluid buildup in the abdomen).
- Efferent Arteriole Vasoconstriction: Renin also causes the efferent arteriole to constrict. While initially this might seem like a way to increase pressure within the glomerulus, in the context of systemic hypotension, this constriction can lead to increased pressure and damage within the kidney itself.
Consequences of Hepatorenal Syndrome
Ultimately, hepatorenal syndrome is characterized by:
- A primary hepatic problem.
- A secondary renal problem driven by vasoconstriction and hypotension.
- The presence of ascites.
- Often, underlying portal hypertension (increased pressure in the portal vein system).
- Damaged kidney tissue and decreased kidney function.
- Elevated levels of blood urea nitrogen (BUN) and creatinine in blood tests, indicating impaired kidney filtration.
Understanding the intricate relationship between the liver and kidneys, and the roles of vasodilation and the renin system, is key to comprehending the development and progression of hepatorenal syndrome.
Shop related blood tests
Read next
 Written on 01/22/2025
Written on 01/22/2025Parkinson's and Huntington's Disease: How Do Dopamine and GABA Imbalances Affect Movement?
Understanding neurological disorders like Parkinson's and Huntington's disease requires delving into the complex world of neurotransmitters. These diseases, while both impacting movement, stem from distinct imbalances in brain chemistry. Read more
 Written on 02/22/2025
Written on 02/22/2025What Is Tinnitus? Causes and Treatment
Tinnitus is a perception of noise or ringing in the ears or head when there is no external source of sound. Read more
 Written on 02/01/2025
Written on 02/01/2025How Does Erythropoiesis Work? Understanding Red Blood Cell Formation, Iron, B12, and Folate's Role in Anemia and Polycythemia.
Erythropoiesis, the process of red blood cell (RBC) formation, is essential for maintaining oxygen transport throughout the body. This intricate process involves multiple factors, including erythropoietin (EPO), iron, vitamin B12, and folate. Understanding these components is crucial for comprehending conditions like anemia and polycythemia. Read more
 Written on 03/07/2025
Written on 03/07/2025What Are Centromeres and Telomeres? Exploring Their Structure, Function, and Role in DNA Replication and Cell Aging.
Ever wondered how our genetic material, DNA, is organized and protected within our cells? Two key structures play vital roles in this process: centromeres and telomeres. Let's dive into their fascinating world and understand their significance in cell division and the aging process. Read more