Constrictive Pericarditis: How Does a Thickened Pericardium Impair Heart Function and Cause Systemic Symptoms Like JVD, Ascites, and Pulsus Paradoxus?
Published on 02/24/2025 · 10 min readThe heart, our tireless engine, is enveloped by a protective sac called the pericardium. Normally thin and flexible, the pericardium can sometimes become thick and rigid due to inflammation, a condition known as pericarditis. When this thickening becomes chronic and constricting, it leads to constrictive pericarditis, significantly hindering the heart's ability to function properly.
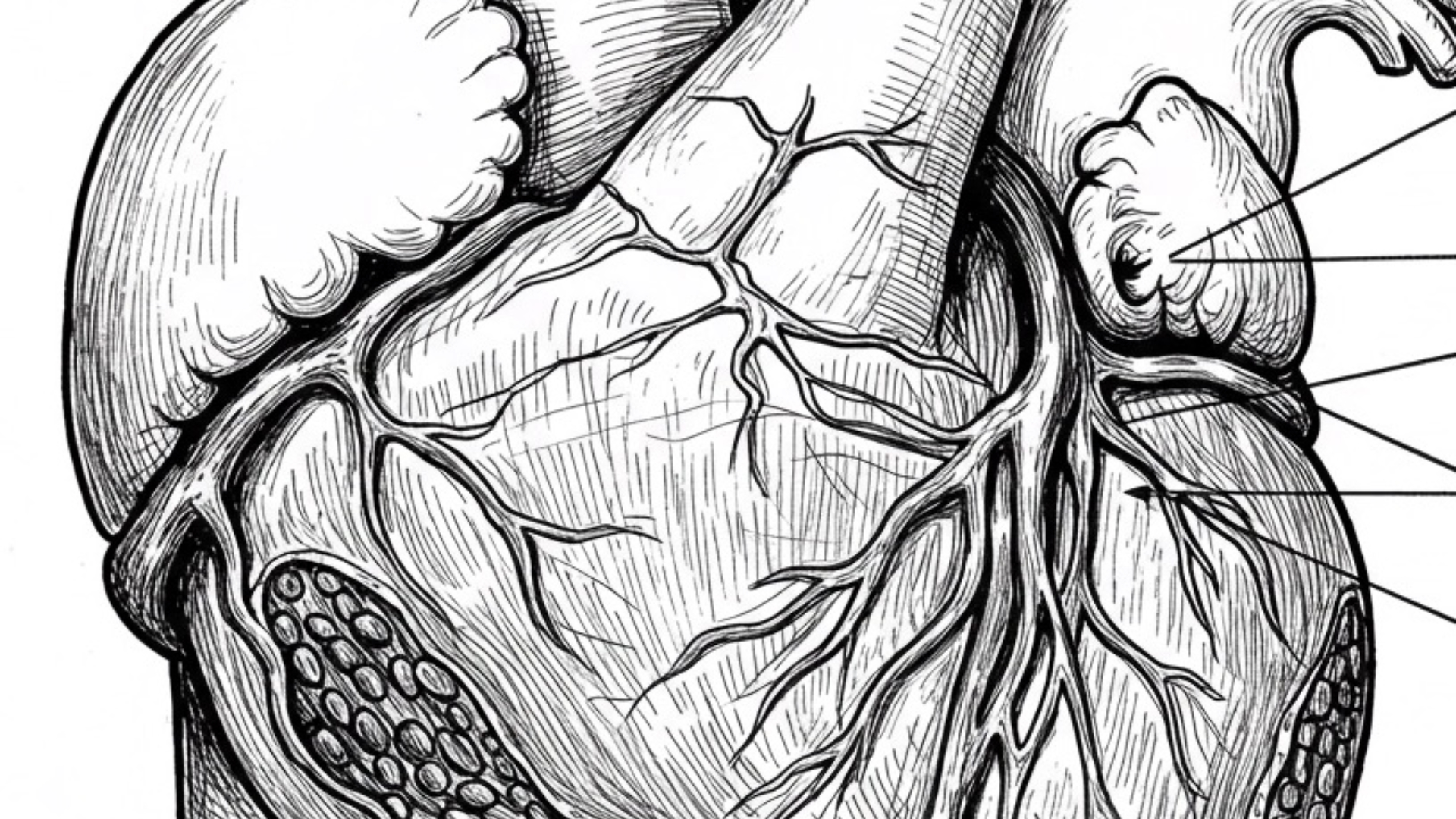
Table of Contents
Understanding Constrictive PericarditisImpact on Right-Sided Heart FunctionImpact on Left-Sided Heart FunctionKey Signs and SymptomsCommon Causes of Constrictive PericarditisDiagnosisTreatmentPrognosis
Understanding Constrictive Pericarditis
In constrictive pericarditis, the heart is essentially trapped within a hardened, often calcified pericardium. This rigid shell prevents the ventricles, the heart's main pumping chambers, from fully relaxing and filling with blood during diastole (the relaxation phase). This impaired diastolic filling leads to a cascade of consequences affecting both the right and left sides of the heart.
Impact on Right-Sided Heart Function
The inability of the right ventricle to relax and accept blood leads to a backup of blood in the right atrium and the systemic venous system. This manifests as:
- Jugular Venous Distension (JVD): Increased pressure in the superior vena cava causes the neck veins to become visibly distended.
- Hepatic Congestion: Blood backs up into the liver, causing it to become enlarged and tender.
- Portal Hypertension: Prolonged hepatic congestion can lead to increased pressure in the portal vein.
- Ascites: Fluid accumulation in the abdominal cavity, often occurring before lower extremity edema in this condition (ascites precox).
- Kussmaul's Sign: An unexpected rise in jugular venous pressure during inspiration. Normally, inspiration decreases intrathoracic pressure, facilitating venous return and causing neck veins to empty. In constrictive pericarditis, the stiff pericardium prevents the right ventricle from accommodating the increased blood flow, leading to venous congestion.
- Proteinuria: Congestion in the inferior vena cava can sometimes affect renal venous drainage, potentially leading to protein in the urine.
Impact on Left-Sided Heart Function
Similarly, the constricted left ventricle struggles to fill adequately, resulting in decreased cardiac output and a backup of blood into the pulmonary circulation. This can lead to:
- Pulmonary Congestion and Pleural Effusion: Back pressure in the pulmonary veins can cause fluid to leak into the lungs (pulmonary edema) and the pleural space (pleural effusion).
- Symptoms of Low Cardiac Output: Fatigue, weakness, and dizziness due to the heart's reduced ability to pump blood effectively.
- Pulsus Paradoxus: An exaggeration of the normal inspiratory drop in systolic blood pressure (greater than 10 mmHg). During inspiration, the increased blood return to the right ventricle can cause it to bulge into the left ventricle due to the fixed pericardial volume, further reducing left ventricular filling and output.
Key Signs and Symptoms
- Jugular Venous Distension (JVD)
- Ascites (often precox)
- Kussmaul's Sign
- Pulsus Paradoxus
- Fatigue and Weakness
- Shortness of Breath
- Peripheral Edema (later in the course)
- Pericardial Knock: An abnormal third heart sound heard during diastole due to the abrupt cessation of ventricular filling by the rigid pericardium.
Common Causes of Constrictive Pericarditis
Several factors can lead to the chronic inflammation and thickening of the pericardium:
- Tuberculosis (TB): A significant infectious cause.
- Post-Cardiac Surgery: Inflammation following heart surgery.
- Post-Radiation Therapy: Radiation exposure to the chest area.
- Other infections (viral, fungal)
- Autoimmune diseases (e.g., lupus, rheumatoid arthritis)
- Uremia (kidney failure)
- Idiopathic (unknown cause)
Diagnosis
Diagnosing constrictive pericarditis involves a combination of clinical evaluation and various diagnostic tests:
- Physical Examination: Assessing for JVD, ascites, Kussmaul's sign, and the presence of a pericardial knock.
- Chest X-ray or CT Scan: May reveal thickening and calcification of the pericardium (water bottle sign on X-ray).
- Echocardiogram: Can show a thickened pericardium, abnormal ventricular filling patterns, and paradoxical septal motion.
- Cardiac MRI: Provides detailed imaging of the pericardium, assessing its thickness and any adhesions.
- Cardiac Catheterization: Can measure pressures in different heart chambers, revealing equalization of diastolic pressures, and demonstrate the characteristic "square root sign" on the right atrial pressure tracing, reflecting rapid early diastolic filling followed by a plateau due to the rigid pericardium.
Treatment
The primary treatment for constrictive pericarditis is surgical pericardiectomy, the surgical removal of the thickened and calcified pericardium. This allows the heart to expand and fill normally. Medical management focuses on treating symptoms and underlying conditions.
Prognosis
The prognosis after pericardiectomy can be good, especially if performed before significant myocardial damage occurs. However, outcomes can vary depending on the underlying cause and the patient's overall health.
Understanding constrictive pericarditis and its diverse manifestations is crucial for timely diagnosis and appropriate management, ultimately improving patient outcomes.
Shop related blood tests
B-Type Natriuretic Peptide (BNP)
While BNP is typically elevated in heart failure due to ventricular stretch, in pure constrictive pericarditis without significant myocardial involvement, BNP levels might be normal or only mildly elevated. Measuring BNP can help differentiate constrictive pericarditis from restrictive cardiomyopathy, where BNP levels are often significantly higher. This distinction is crucial as they can present with similar symptoms.
CRP is a marker of inflammation in the body. While constrictive pericarditis is a result of chronic inflammation, a significantly elevated CRP might suggest an ongoing active inflammatory process or an underlying inflammatory condition that could have led to the pericarditis (though it's not specific to the pericardium). It can provide context but isn't diagnostic for constrictive pericarditis itself.
These tests can help assess for signs of systemic congestion and potential liver involvement, as discussed in the blog post (hepatic congestion leading to potential protein abnormalities). While not specific to constrictive pericarditis, changes in these levels can support the clinical picture of systemic venous congestion. Additionally, significantly low albumin could point towards other underlying conditions.
Read next
 Written on 02/07/2025
Written on 02/07/2025What is ANCA-associated vasculitis, how does it damage blood vessels, and what are the key treatments for this autoimmune condition?
ANCA-associated vasculitis is a group of autoimmune diseases characterized by inflammation of small and medium-sized blood vessels. This inflammation, or vasculitis, can lead to significant damage, potentially causing tissue ischemia and aneurysms. The presence of anti-neutrophil cytoplasmic antibodies (ANCA) in the blood is a hallmark of these conditions. Read more
 Written on 02/13/2025
Written on 02/13/2025How does plasminogen activator inhibitor (PAI) regulate fibrinolysis and what are the clinical implications of PAI deficiency or excess?
Fibrinolysis, the process of breaking down blood clots, is a crucial part of hemostasis. Plasminogen activator inhibitor (PAI) plays a vital role in regulating this process. Understanding PAI's function and its clinical implications is essential for comprehending bleeding and coagulation disorders. Read more
 Written on 03/02/2025
Written on 03/02/2025What is Korsakoff Syndrome, its causes including thiamine deficiency and alcoholism, key symptoms like amnesia and confabulation, affected brain regions, diagnosis, and treatment with vitamin B1?
Ever wondered about a condition that intricately links memory, nutrition, and even excessive alcohol consumption? Let's dive into Korsakoff Syndrome, a fascinating yet serious neurological disorder. Read more
 Written on 02/26/2025
Written on 02/26/2025What Are Common Quadriceps Injuries Like Strains and Contusions, How Do They Happen, What Are the Symptoms, and What Are the Treatment Approaches?
The quadriceps are a powerful group of four muscles located in the front of your thigh. They play a crucial role in extending your knee and, in the case of the rectus femoris, also assist with hip flexion. Unfortunately, these strong muscles are susceptible to injury, particularly during sports and activities involving sprinting, jumping, and sudden changes in direction. Read more