Streptococcus Pneumoniae: How Do You Diagnose and Treat This Bacterial Infection?
Published on 01/08/2025 · 7 min readStreptococcus pneumoniae is a common yet potentially serious bacterial pathogen. Understanding its diagnosis and treatment is crucial for effective patient care. This blog post will delve into the key aspects of identifying and managing Streptococcus pneumoniae infections.
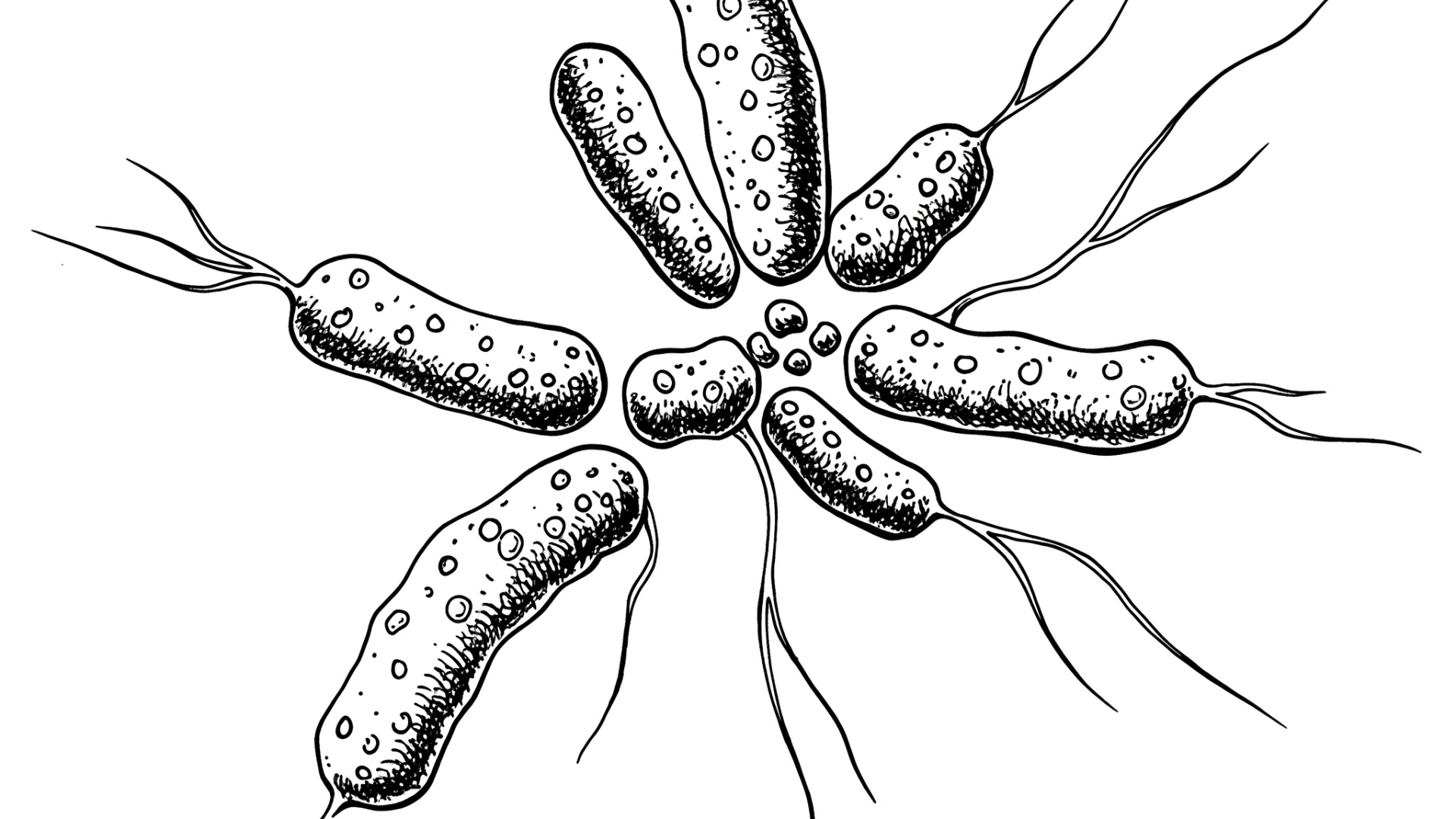
Table of Contents
What is Streptococcus Pneumoniae?Key CharacteristicsDiseases Caused by Streptococcus PneumoniaeHow is Streptococcus Pneumoniae Diagnosed?MicroscopyCultureNucleic Acid Amplification Tests (NAAT)IdentificationTreatment of Streptococcus Pneumoniae InfectionsOutpatient TherapyInpatient TherapyVaccinationPrevention
What is Streptococcus Pneumoniae?
Streptococcus pneumoniae is a gram-positive, catalase-negative, alpha-hemolytic bacterium. It often appears as diplococci (pairs) or short chains under a microscope. Key characteristics include sensitivity to optochin and solubility in bile. It's encapsulated, with the capsule being its most significant virulence factor.
Key Characteristics:
- Gram-positive cocci
- Catalase-negative
- Alpha-hemolytic
- Optochin-sensitive
- Bile-soluble
- Encapsulated
Diseases Caused by Streptococcus Pneumoniae
This bacterium can cause a range of infections, including:
- Meningitis: Inflammation of the meninges.
- Otitis Media: Middle ear infection.
- Pneumonia: Lung infection.
- Sinusitis: Sinus infection.
- Bacteremia: Bloodstream infection (often associated with meningitis and pneumonia).
How is Streptococcus Pneumoniae Diagnosed?
Diagnosis involves several methods:
Microscopy
Gram staining of samples (e.g., cerebrospinal fluid, sputum) reveals gram-positive diplococci or short chains surrounded by a capsule. Older cultures may stain poorly. A Quellung reaction can confirm the presence of the capsule.
Culture
Streptococcus pneumoniae requires enriched media supplemented with blood products. Samples should be collected before antibiotic administration. Blood cultures are useful in cases of bacteremia, meningitis, and pneumonia.
Nucleic Acid Amplification Tests (NAAT)
NAATs offer rapid detection of bacterial DNA but are less commonly used in clinical practice for this specific organism.
Identification
Biochemical tests, such as optochin sensitivity and bile solubility, help identify the bacteria. Antigen detection, especially for pneumococcal C polysaccharide, can also be useful.
Treatment of Streptococcus Pneumoniae Infections
Treatment strategies vary based on the severity and location of the infection:
Outpatient Therapy
For outpatients without modifying factors (e.g., age >65, recent antibiotic use), macrolides like azithromycin or clarithromycin are often used. If modifying factors are present, respiratory quinolones (e.g., levofloxacin) or beta-lactams (e.g., amoxicillin-clavulanate, cefpodoxime, cefuroxime) plus a macrolide may be prescribed.
Inpatient Therapy
For hospitalized patients not in the ICU, treatment mirrors that of outpatients with modifying factors. ICU patients require more aggressive therapy, typically involving a respiratory quinolone plus a beta-lactam. Vancomycin may be added if MRSA is suspected. Antipseudomonal antibiotics are added if pseudomonas is suspected and a neuraminidase inhibitor if influenza is suspected.
Vaccination
Two types of pneumococcal vaccines are available: the 23-valent pneumococcal polysaccharide vaccine (PPSV23) and the 13-valent pneumococcal conjugate vaccine (PCV13). PCV13, being conjugated, provides stronger and longer-lasting immunity by activating T-lymphocytes.
Prevention
Prevention includes avoiding contact with sick individuals and vaccination. Understanding the risk factors and taking appropriate preventive measures can significantly reduce the incidence of Streptococcus pneumoniae infections.
Shop related blood tests

Complete Blood Count (CBC) with Differential and Platelets Blood Test
A complete blood count is essential for assessing the overall health of the patient and detecting signs of infection, such as an elevated white blood cell count.
Read next
 Written on 02/04/2025
Written on 02/04/2025Leukemoid Reaction vs. CML: How to Differentiate and When to Suspect Each Condition?
Understanding the difference between a leukemoid reaction and chronic myelogenous leukemia (CML) is crucial for accurate diagnosis and appropriate patient management. This blog post will delve into the key distinctions, causes, and diagnostic approaches for these two conditions. Read more
 Written on 01/29/2025
Written on 01/29/2025Phenytoin: How does it work, what are its side effects, and what is fetal hydantoin syndrome?
Phenytoin is a widely used antiepileptic medication, but understanding its mechanism, side effects, and potential risks, like fetal hydantoin syndrome, is crucial. This blog post will break down the key aspects of phenytoin. Read more
 Written on 02/23/2025
Written on 02/23/2025External and Middle Ear Anatomy: How Do Structure and Function Impact Hearing and Common Ear Conditions?
Understanding the anatomy of the external and middle ear is crucial for comprehending how we hear and why certain ear conditions develop. This blog post delves into the key structures and their functions, highlighting common issues like swimmer's ear and eardrum perforation. Read more
 Written on 03/03/2025
Written on 03/03/2025What is Hepatorenal Syndrome? Understanding the Liver-Kidney Connection, Symptoms, and the Role of Vasodilation and Renin?
Let's dive into hepatorenal syndrome, a serious condition where a problem in the liver leads to kidney dysfunction. As the name suggests, hepato refers to the liver, and renal refers to the kidney. Understanding this connection is crucial for recognizing and managing this syndrome. Read more